Approximately 35.3 million of people are infected with the human immunodeficiency virus (HIV) worldwide, and 20–30% of them are also contaminated with the hepatitis C virus (HCV). The introduction of highly active antiretroviral therapy increased the survival time and improved the quality of life of HIV-infected individuals, however hepatic diseases related to chronic HCV infection became the main cause of morbidity and mortality in these patients.1 The present work aimed to study the prevalence and risk factors for HCV infection in a sample of HIV-infected patients from a medium size urban center in the countryside of South Brazil.
Adult individuals with HIV receiving care in a reference outpatient treatment center for HIV testing and AIDS treatment in Cruz Alta (located in the Northwest region of the state of Rio Grande do Sul, Brazil) were consecutively enrolled in the study from July 2011 to August 2012. Socio-demographic and potential risk factors for HIV infection were obtained with a standardized individual questionnaire. General laboratory and clinical data were obtained from the medical records. All participants signed an informed consent form. The study was approved by the Research Ethics Committees of the Universidade Luterana do Brasil.
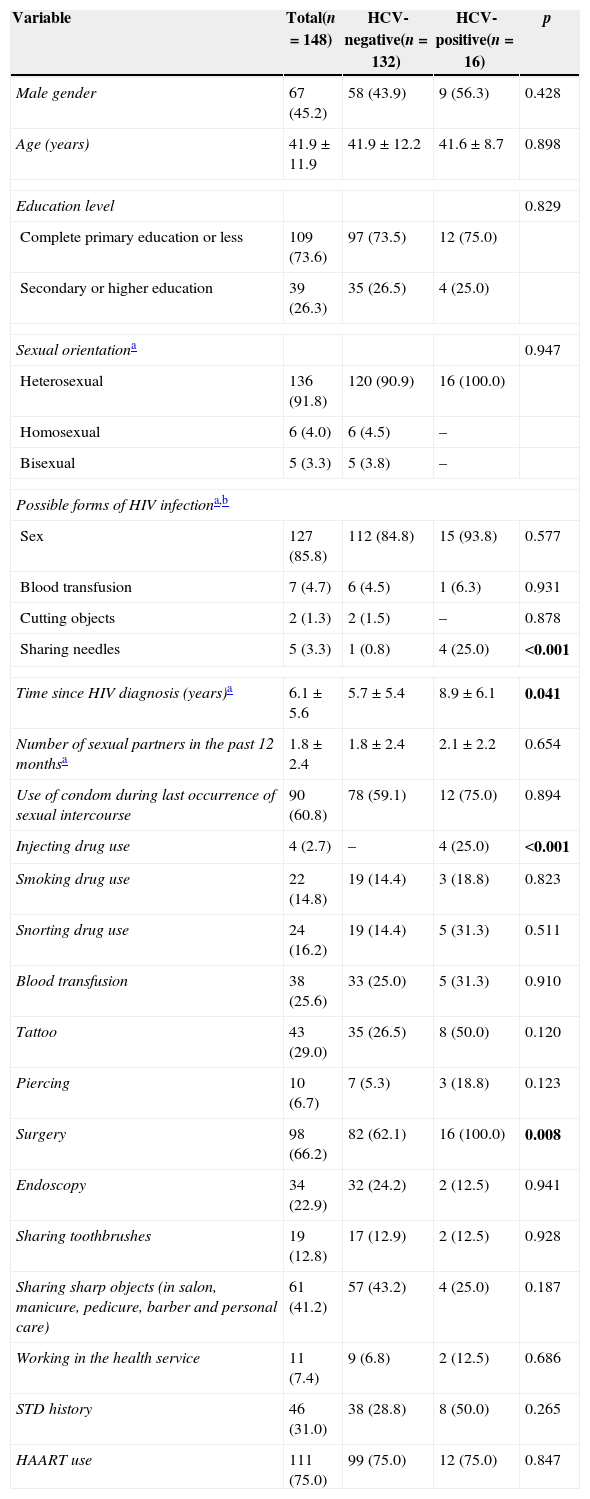
A total of 148 HIV-infected patients were included in the study. Sixteen patients (10.8%) had anti-HCV and HCV-RNA positive results. A total of 13 patients (81.2%) were infected with HCV genotype 1, and three (18.8%) with genotype 3. Use of intravenous drugs and report of possible HIV acquisition by sharing needles were significantly higher in co-infected than in mono-infected patients (p<0.001) (Table 1). The time period since HIV diagnosis was longer in co-infected than in mono-infected patients (p=0.041). A higher proportion of HIV/HCV co-infected patients (100.0%) than mono-infected patients (62.1%) had undergone surgery in the past (p=0.008). In the multivariate analysis, use of injecting drugs (p=0.021), surgery history (p<0.001) and male gender (p<0.001) were the independent risk factors associated with HIV/HCV co-infection.
Distribution of socio-demographic and epidemiological characteristics in HIV-positive patients according to HCV status.
| Variable | Total(n=148) | HCV-negative(n=132) | HCV-positive(n=16) | p |
|---|---|---|---|---|
| Male gender | 67 (45.2) | 58 (43.9) | 9 (56.3) | 0.428 |
| Age (years) | 41.9±11.9 | 41.9±12.2 | 41.6±8.7 | 0.898 |
| Education level | 0.829 | |||
| Complete primary education or less | 109 (73.6) | 97 (73.5) | 12 (75.0) | |
| Secondary or higher education | 39 (26.3) | 35 (26.5) | 4 (25.0) | |
| Sexual orientationa | 0.947 | |||
| Heterosexual | 136 (91.8) | 120 (90.9) | 16 (100.0) | |
| Homosexual | 6 (4.0) | 6 (4.5) | – | |
| Bisexual | 5 (3.3) | 5 (3.8) | – | |
| Possible forms of HIV infectiona,b | ||||
| Sex | 127 (85.8) | 112 (84.8) | 15 (93.8) | 0.577 |
| Blood transfusion | 7 (4.7) | 6 (4.5) | 1 (6.3) | 0.931 |
| Cutting objects | 2 (1.3) | 2 (1.5) | – | 0.878 |
| Sharing needles | 5 (3.3) | 1 (0.8) | 4 (25.0) | <0.001 |
| Time since HIV diagnosis (years)a | 6.1±5.6 | 5.7±5.4 | 8.9±6.1 | 0.041 |
| Number of sexual partners in the past 12 monthsa | 1.8±2.4 | 1.8±2.4 | 2.1±2.2 | 0.654 |
| Use of condom during last occurrence of sexual intercourse | 90 (60.8) | 78 (59.1) | 12 (75.0) | 0.894 |
| Injecting drug use | 4 (2.7) | – | 4 (25.0) | <0.001 |
| Smoking drug use | 22 (14.8) | 19 (14.4) | 3 (18.8) | 0.823 |
| Snorting drug use | 24 (16.2) | 19 (14.4) | 5 (31.3) | 0.511 |
| Blood transfusion | 38 (25.6) | 33 (25.0) | 5 (31.3) | 0.910 |
| Tattoo | 43 (29.0) | 35 (26.5) | 8 (50.0) | 0.120 |
| Piercing | 10 (6.7) | 7 (5.3) | 3 (18.8) | 0.123 |
| Surgery | 98 (66.2) | 82 (62.1) | 16 (100.0) | 0.008 |
| Endoscopy | 34 (22.9) | 32 (24.2) | 2 (12.5) | 0.941 |
| Sharing toothbrushes | 19 (12.8) | 17 (12.9) | 2 (12.5) | 0.928 |
| Sharing sharp objects (in salon, manicure, pedicure, barber and personal care) | 61 (41.2) | 57 (43.2) | 4 (25.0) | 0.187 |
| Working in the health service | 11 (7.4) | 9 (6.8) | 2 (12.5) | 0.686 |
| STD history | 46 (31.0) | 38 (28.8) | 8 (50.0) | 0.265 |
| HAART use | 111 (75.0) | 99 (75.0) | 12 (75.0) | 0.847 |
Note: Variables expressed as number (percentage) or mean±standard deviation.
STD, sex transmitted disease; HAART, highly active antiretroviral therapy.
Bold values are those statistically significant (p<0.05), but this emphasis can be omitted.
The prevalence of HIV/HCV co-infection varies with the geographic region. In Brazil, reports estimated an average of 20.3% of HIV/HCV co-infection, ranging from 3.3% to 82.4% according to the region.2 Epidemiological studies conducted in the capital cities and metropolitan regions from Brazil have demonstrated high HIV/HCV co-infection, mainly associated to injecting drug use.2 However, epidemiological reports are sparse from the countryside, limiting a better understanding of these epidemiological aspects in Brazil. The present study focused in the city of Cruz Alta, a medium size urban center with one of the highest incidence rate of HIV/AIDS in Rio Grande do Sul.3 HIV/HCV co-infection frequency was lower than in the two cities of the metropolitan area of the state, Porto Alegre (31.2%) and Canoas (23.8%).4,5 Interestingly the frequency of injecting drug users was also lower in the investigated population (2.7%) than those reported in other studies.4,5 The low HIV/HCV co-infection prevalence is probably related to the low frequency of injecting drug users in the community. This epidemiologic knowledge is essential for the development of specific prevention strategies in small and medium size cities from the Brazilian countryside.
Conflicts of interestThe authors declare no conflicts of interest.
The authors would like to thank the patients and staff of the Specialized Service (SAE) of Cruz Alta, RS, for their collaboration in the development of this study.