Hepatitis C virus (HCV) infection is associated with numerous extrahepatic manifestations.1 Very little is known about the prevalence of these manifestations in Brazil, a country where 1.4% of the population (nearly 2.6 million people) is infected.2 After Ethics Committee approval, between August 2009 and December 2013 we consecutively enrolled untreated patients aged 18 years or more who tested positive for HCV-RNA, excluding cases co-infected with HIV or hepatitis B. We obtained medical history with a standardized questionnaire, and performed physical examination, and blood and urine tests. We evaluated patients for the presence of arthralgia, myalgia, fatigue, pruritus, palpable purpura, vasculitis, sicca symptoms, thyroid dysfunction, diabetes mellitus, psoriasis, lichen planus, porphyria cutanea tarda, renal impairment, thrombocytopenia, cryoglobulinemia, and paresthesia. All patients had a liver biopsy, and histological abnormalities were graded using the Metavir system. We estimated the prevalence of extrahepatic manifestations and used logistic regression models to assess the combined influence of patient and virus characteristics on selected manifestations. We assessed 190 patients with a mean age of 48 years, 59% were females, and HCV genotypes were 1 and 3 in 77% and 19% of cases, respectively. A history of exposure was reported by 51% of patients, alcohol consumption was <20g/day in 84%, and 73% had a history of <15 pack-years of smoking. Fibrosis scores were F0/1/2/3/4 in 25%, 48%, 20%, 5%, and 3%, respectively. At least one extrahepatic manifestation was present in 79% of patients, the most frequent being arthralgia (57%), myalgia (50%), fatigue (48%), sicca symptoms (15%; 22 patients had xerophthalmia, 14 had xerostomia, and six had both), hypothyroidism (12%), and thrombocytopenia (10%). Although all patients were tested, only two had cryoglobulinemia. Table 1 shows the results of the multivariate analyses, considering only extrahepatic manifestations for which at least one patient or viral feature was predictive in univariate analysis. Gender and age were the baseline patient features more often associated with extrahepatic manifestations. Except for thrombocytopenia, which was significantly more frequent in males, the other manifestations were more frequent in females. The only significant non-demographic feature in this analysis was the presence of grade 3 or 4 fibrosis, which was associated with thrombocytopenia. Although a high prevalence of musculoskeletal complaints has been documented in patients with hepatitis C,3–5 we found rates of arthralgia and myalgia which are on the upper end of the range reported in the literature, perhaps due to our proactive search for these symptoms. Our results suggest that extrahepatic manifestations are more frequent in females, and many are significantly associated with older age. This is one of the few studies that analyzed extrahepatic manifestations in consecutive HCV patients, most of which without cryoglobulinemia. We believe that the low prevalence of mixed cryoglobulinemia is related to the referral of patients to other services and not due to error in detecting cryoglobulins. Further studies are needed to better understand the natural history and to determine the best therapeutic approach for patients with these comorbidities.
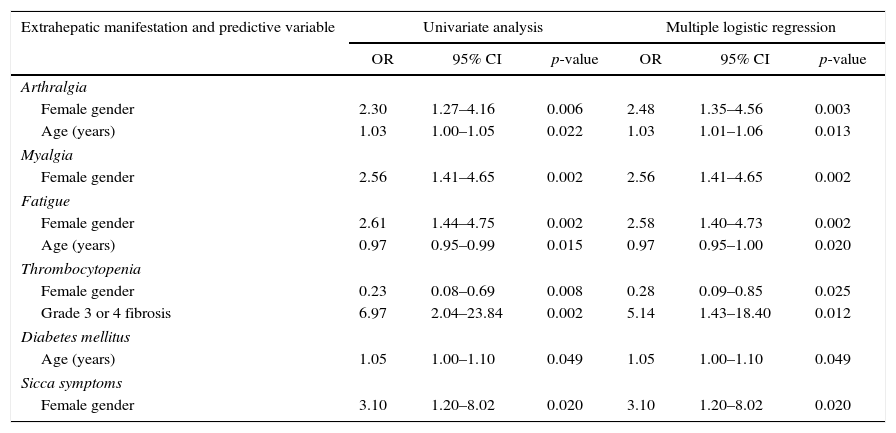
Univariate and multivariate logistic regression analyses of potential correlates of various extrahepatic manifestations.
| Extrahepatic manifestation and predictive variable | Univariate analysis | Multiple logistic regression | ||||
|---|---|---|---|---|---|---|
| OR | 95% CI | p-value | OR | 95% CI | p-value | |
| Arthralgia | ||||||
| Female gender | 2.30 | 1.27–4.16 | 0.006 | 2.48 | 1.35–4.56 | 0.003 |
| Age (years) | 1.03 | 1.00–1.05 | 0.022 | 1.03 | 1.01–1.06 | 0.013 |
| Myalgia | ||||||
| Female gender | 2.56 | 1.41–4.65 | 0.002 | 2.56 | 1.41–4.65 | 0.002 |
| Fatigue | ||||||
| Female gender | 2.61 | 1.44–4.75 | 0.002 | 2.58 | 1.40–4.73 | 0.002 |
| Age (years) | 0.97 | 0.95–0.99 | 0.015 | 0.97 | 0.95–1.00 | 0.020 |
| Thrombocytopenia | ||||||
| Female gender | 0.23 | 0.08–0.69 | 0.008 | 0.28 | 0.09–0.85 | 0.025 |
| Grade 3 or 4 fibrosis | 6.97 | 2.04–23.84 | 0.002 | 5.14 | 1.43–18.40 | 0.012 |
| Diabetes mellitus | ||||||
| Age (years) | 1.05 | 1.00–1.10 | 0.049 | 1.05 | 1.00–1.10 | 0.049 |
| Sicca symptoms | ||||||
| Female gender | 3.10 | 1.20–8.02 | 0.020 | 3.10 | 1.20–8.02 | 0.020 |
CI, confidence interval; OR, odds ratio.
The authors declare no conflicts of interest.