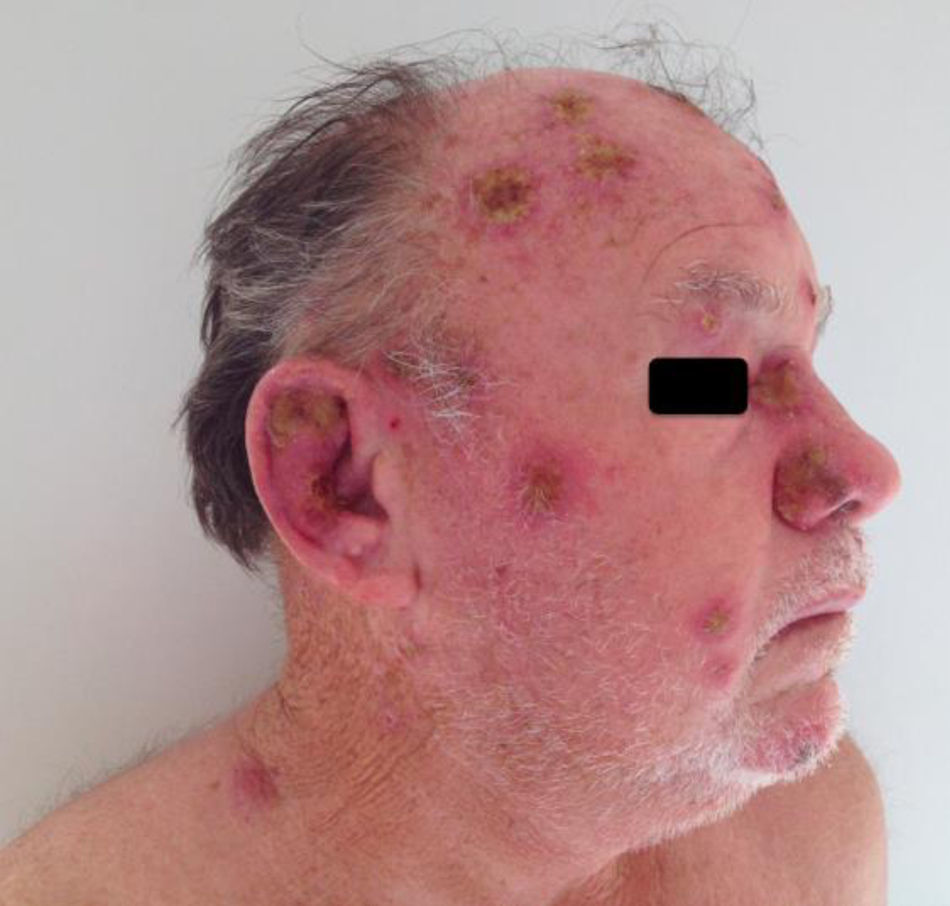
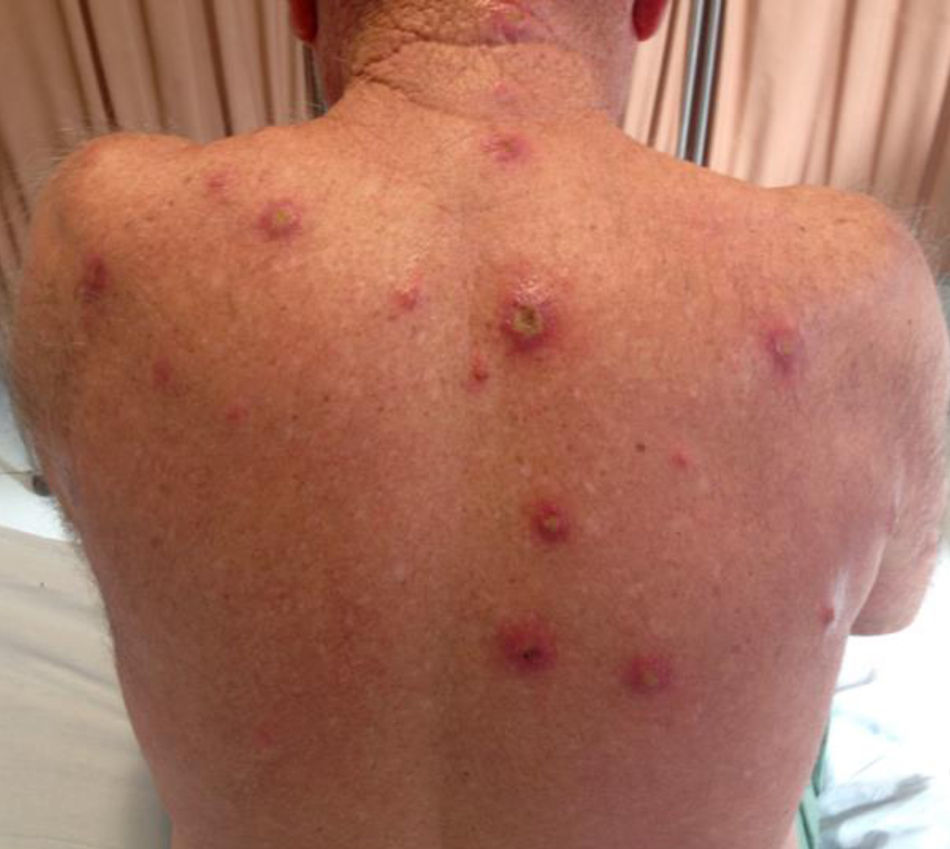
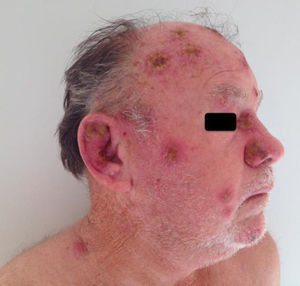
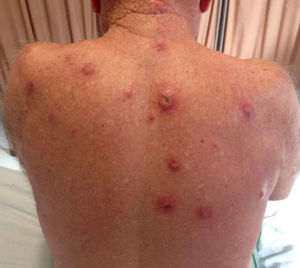
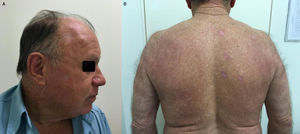
A 69-year-old male patient, with history of multiple furuncles for two months, without improvement after the use of cephalexin and amoxicillin/clavulanate for 20 days, and daily fever for a week. On dermatological examination, multiple ulcerovegetative and ulcero-crusted cutaneous lesions on the face, ears, scalp, back, upper and lower limbs and genitalia were observed (Figs. 1 and 2). There was no lymphadenopathy. Based on the clinical picture the hypotheses of disseminated cutaneous leishmaniasis, paracoccidioidomycosis, and malignant syphilis were raised. Laboratory tests (blood count, renal function, hepatography, and coagulogram) were normal. Serology for hepatitis, syphilis, HIV, and Leishmania donovani were negative.
Swabs taken from open lesions for direct mycological examination and culture for fungi were negative. Histopathological of the edge of an ulcer on the dorsum demonstrated dense lymphohistiocytic inflammatory infiltrate with plasma and mast cells, in addition to neutrophils and granuloma formation; hyperplastic skin surrounded with areas of pseudoepitheliomatous pattern. Giemsa and Ziehl-Neelsen staining were negative for fungi and acid-fast bacilli, respectively. Rounded and oval structures with kinetoplast, phagocytosed in macrophages were observed.
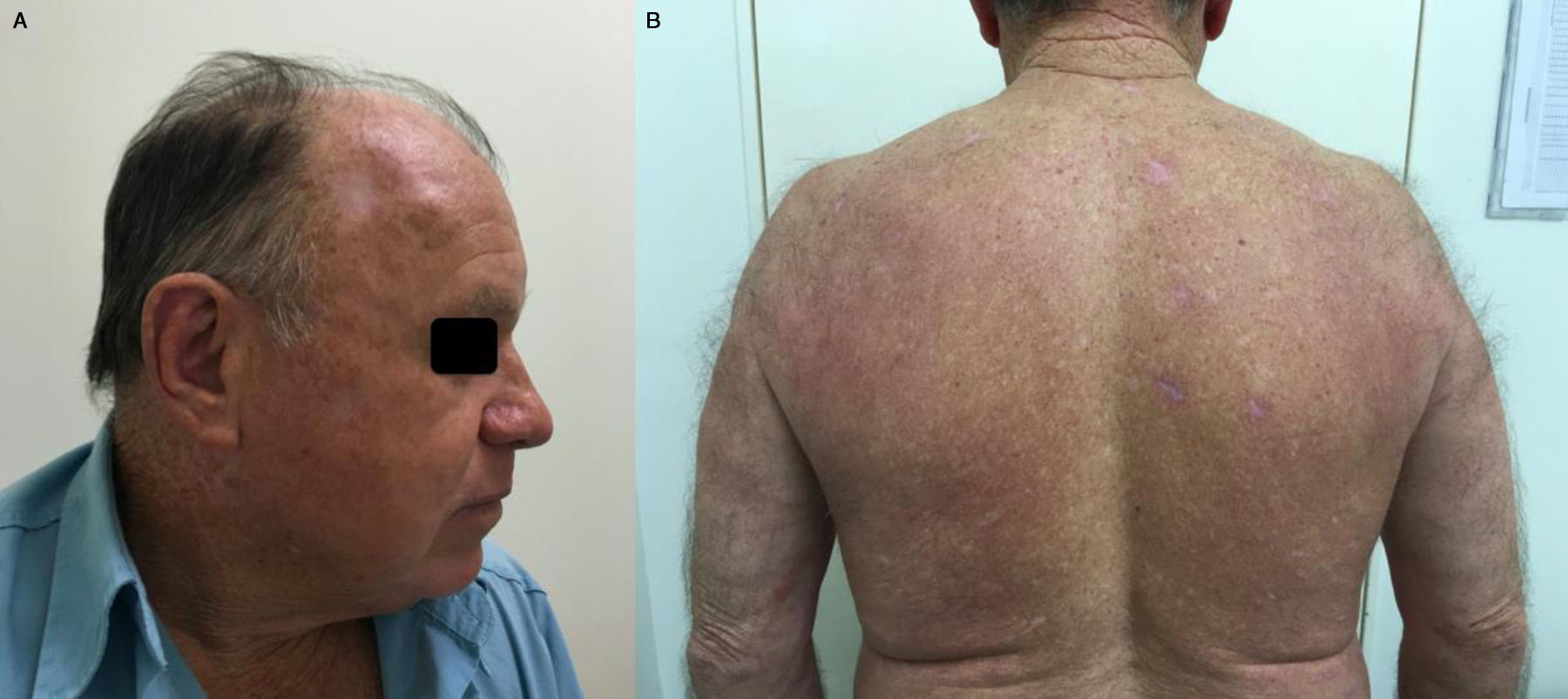
Based on clinical and histological picture of chronic ulcerated dermatitis associated with leishmanias, the diagnosis of disseminated cutaneous leishmaniasis was established, the treatment with meglumine antimoniate 20mg/kg/day was started, and administered for 30 days. After 20 days of the end of treatment, there was healing of skin and mucosal lesions. He is in the ninth month of follow-up, with no appearance of new lesions and complications (Fig. 3).
A negative serology for L. donovani came as no surprise, as this agent causes visceral leishmaniasis, with rare cases of skin lesions described in the literature.1,2 Currently considered an emerging form of the disease,3 disseminated leishmaniasis should be detected early, recognizing its clinical spectrum and disabling potential.
Conflicts of interestThe authors declare no conflicts of interest.