Here we report the case of a patient who developed urinary tract infection after a urodynamic study. The causative agent was Raoultella planticola, a rare opportunistic pathogen that usually invades immunocompromised patients. While a urinary tract infection with R. planticola has been previously described, this is the first report in which an R. planticola infection developed after a urodynamic study. We postulate that the mechanism of infection was direct invasion of the urinary tract from contaminated urodynamic study equipment. Here, we discuss the role played by isotonic solutions in facilitating bacterial reproduction.
Both lower urinary tract and pelvic floor function can be efficiently evaluated by a urodynamic study (US),1 but it is an invasive procedure that involves urethral catheterization. A urinary tract infection (UTI) is the most frequent complication.2 In patients undergoing a US, however, infection due to contamination of the equipment used in the evaluation is unusual. Herein we present a case of hospital-acquired UTI resulting from infection with Raoultella planticola in a patient who underwent a US prior to kidney transplantation. R. planticola is a Gram-negative bacterium that usually invades immunocompromised patients and sometimes causes serious infections. To our knowledge, this is the first case of a UTI caused by R. planticola that occurred subsequent to a US.
Case presentationA 57-year-old male who had been on peritoneal dialysis for the past two years because of end-stage renal disease secondary to diabetes mellitus was admitted to our clinic for a live kidney transplant. The results of the basic investigations used to determine transplant eligibility did not reveal any obstacles to transplantation. However, urodynamic testing (voiding pressure-flow analysis) was performed because he complained of problems in initiating urination; these were attributed to benign prostatic hypertrophy, identified on ultrasonography (USG). One day after the US, the patient complained of dysuria, and then, three days after, of fever and chills. On physical examination, his general condition was moderate and he had a blood pressure of 140/70mmHg, a heart rate of 110beats/min, a respiratory rate of 17breaths/min, and his body temperature was 37.8°C. The only significant physical finding was suprapubic tenderness. His white blood cell count was 17,400cells/μL (absolute neutrophil count, 14,880cells/μL), and urinalysis showed a high number of white blood cells and erythrocytes. His biochemical test results were as follows: plasma creatinine 10.3mg/dL, blood urea nitrogen 86mg/dL, sodium 133mEq/dL, potassium 4.7mEq/dL, and C-reactive protein (CRP) 75mg/L (reference range, 0–5mg/L). The peritoneal fluid cell count was 10/mm3. A chest X-ray was unremarkable. USG of the pelvis identified only bladder wall thickness. Two peripheral blood cultures, a peritoneal fluid culture and a urinary culture were taken. The patient was treated with empirical broad-spectrum intravenous antibiotic therapy (ceftriaxone, 1g q12h) for the UTI after the first evaluation. The urine culture revealed R. planticola, but his blood cultures and peritoneal fluid culture turned out negative.
We suspected that the infection was secondary to bacterial invasion from contaminated US equipment because R. planticola is a rare causative bacteria for UTI and therefore set up cultures from samplings of the different parts of the device. Both the culture from the US pump tube and the isotonic solution were positive for R. planticola; moreover, the strain was identical to that isolated from the patient's urine. During the second day of antibiotic treatment, the patient's clinical condition improved significantly. His serum CRP level decreased to 5mg/L; on day 7 of treatment, his WBC was 8700/mm3. Ceftriaxone therapy was therefore stopped. He was transplanted with a live kidney one month later.
DiagnosisA urine specimen was sent to the microbiology department for culture. Gram-negative rods and polymorphonuclear leukocytes were seen in the Gram-stained sample. The urine sample was cultivated on EMB and sheep blood agar with a 10-μL standard loop as the inoculant. Gram-negative bacilli grew on both culture media to a density of >100,000CFU/mL. The isolate was analyzed by matrix-assisted laser desorption/ionization time-of-flight mass spectrometry using the VITEK MS (bioMérieux, Marcy l’Étoile, France) system and identified as R. planticola. Antimicrobial susceptibility testing was performed using the VITEK-2 compact system. The bacterium was resistant to ampicillin and fosfomycin and susceptible to amoxicillin/clavulanic acid, ceftriaxone, ciprofloxacin, gentamicin, ceftazidime, cefuroxime axetil, trimethoprim/sulfamethoxazole, and nitrofurantoin (Table 1). The culture from the US pump tube and isotonic solution revealed the same strain of R. planticola as isolated from the patient's urine. The results were interpreted according to the guidelines of the European Committee on Antimicrobial Susceptibility Testing.
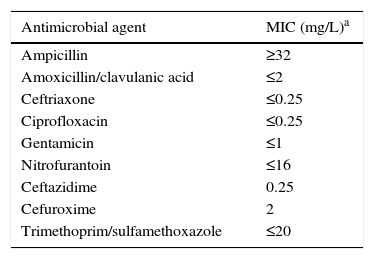
In vitro susceptibility results for Raoultella planticola (urine, US pump, and isotonic solution).
| Antimicrobial agent | MIC (mg/L)a |
|---|---|
| Ampicillin | ≥32 |
| Amoxicillin/clavulanic acid | ≤2 |
| Ceftriaxone | ≤0.25 |
| Ciprofloxacin | ≤0.25 |
| Gentamicin | ≤1 |
| Nitrofurantoin | ≤16 |
| Ceftazidime | 0.25 |
| Cefuroxime | 2 |
| Trimethoprim/sulfamethoxazole | ≤20 |
MIC, minimum inhibitory concentration.
R. planticola is a Gram-negative, non-motile, encapsulated bacterium previously referred to as Klebsiella planticola but reclassified as a new genus in 2001.3 Although R. planticola is mainly an aquatic and soil bacterium, it has been clinically isolated from human sputum, stool, wounds, and urine.4,5 To date, several human infections with R. planticola have been reported. Risk factors for these infections include immunosuppression, comorbidities, and invasive procedures.6,7
R. planticola may also cause UTIs.8,9 In our patient, diabetes and chronic renal failure were the major comorbidities, which led to an immunosuppressed state. An additional risk factor was the invasive procedure he underwent, US, which requires urethral catheterization. The most common complication after a US is UTI10; however, in these cases the most frequently isolated causative agent is Escherichia coli, with pathogens such as Klebsiella species or members of the Enterobacteriaceae encountered only rarely.11,12 To our knowledge, this is the first case of an R. planticola infection that developed subsequent to a US.
In our unit, a sterile isotonic solution is used for a US, and the pump tube is replaced every three days. There were no previous incidences of UTI due to contamination of the test device. However, after the urine culture revealed R. planticola, the infection was regarded as contamination in its origin. This was confirmed by the finding that the US pump tube and isotonic solution were contaminated with the same strain of R. platicola isolated from the patient. Bacterial contamination of US equipment was previously reported.13 In our investigation of the source of the contamination, we established that the isotonic solution had been opened for use in another patient in the previous week and should have been discarded thereafter; instead, it was mistakenly used in our patient. Isotonic solutions may be contaminated by contact with another infected patient or by bacterial transmission from the environment, including via surface contact, invasive procedures, and as a bioaerosol through the air.14
Microorganisms such as R. planticola that are commonly found in aquatic environments may be able to rapidly multiply in the isotonic solutions used in US devices. A previous case report described the development of cholangitis caused by R. planticola in a patient who had undergone an endoscopic retrograde cholangiopancreatographic procedure, which also involved the use of an isotonic solution. The cause of the infection in that patient was attributed to an inadequately sterilized, reusable endoscopy line.7
R. planticola is generally sensitive to cephalosporins, aminoglycosides, fluoroquinolones, and carbapenems, but extensive resistance has also been described for this bacterium.15 The isolate from our patient was resistant to ampicillin and fosfomycin, and susceptible to amoxicillin/clavulanic acid, ceftriaxone, ciprofloxacin, gentamicin, ceftazidime, cefuroxime axetil, trimethoprim/sulfamethoxazole, and nitrofurantoin. Treatment with a 1-week course of ceftriaxone (2g/day) resulted in full recovery and abolishment of the infection.
In conclusion, we present the case of a patient who underwent an invasive urinary tract procedure and subsequently developed a UTI, with R. planticola identified as the causative agent. The patient's clinical presentation was consistent with a UTI, determined to be nosocomial, associated with the use of a contaminated isotonic solution. The patient suffered from diabetes and chronic renal failure, both of which may have been contributing factors in the pathogenesis of the infection. Our results emphasize the need for the strict implementation of measures to ensure that US devices, especially the isotonic solution, are properly sterilized prior to their use.
Conflicts of interestThe authors declare no conflicts of interest.