The prevalence of keratoconjunctivitis sicca (KCS) associated with Human T-Cell Lymphotropic Virus Type 1 (HTLV-1) (HTLV-1/KCS) has been estimated at around 37%, but its clinical manifestations are poorly described.
PurposeTo determine the prevalence and associated factors of HTLV-1/KCS in a large cohort of HTLV-1-infected individuals living in Salvador, Brazil.
MethodsA cross-sectional study was conducted between June 2004 and September 2017 at the Integrative and Multidisciplinary Center for HTLV in Salvador, Bahia-Brazil. Data from 758 HTLV-1-infected patients was collected. A complete ophthalmologic examination was performed in both eyes. Lacrimal function was evaluated by breakup time, Rose Bengal and Schirmer I Tests. KCS diagnosis was considered in the presence of at least two out of three positive tests. HTLV-1 proviral load Crude and Adjusted Prevalence Rates (PR) with 95% Confidence Intervals (95% CI) were estimated using multivariate Poisson Regression with robust error variance.
ResultsThe overall prevalence of KCS was 31.7%, with higher rates observed in HTLV-1-associated myelopathy/tropical spastic paraparesis patients (crude PR: 1.84; CI95%: 1.50–2.26) even after adjusting for age, sex, time of HTLV-1 diagnosis and schooling (adjusted PR: 1.63; CI95%: 1.31–2.02). Proviral load, low corrected visual acuity, burning and/or pain and itching were all significantly higher in patients with KCS.
ConclusionBurning and/or pain and itching and low corrected visual acuity were the most common alterations of HTLV-1/KCS. High Proviral load was found to be associated with the presence of KCS. It is strongly recommended that HTLV-1 patients undergo periodic ophthalmologic examination to promote the early diagnosis of KCS and prevent the consequences associated with dry eye disease.
Human T-lymphotropic virus type 1 (HTLV-1) is etiologically linked with adult T cell leukemia (ATL),1 tropical spastic paraparesis/HTLV-1-associated myelopathy (HAM/TSP),2,3 infective dermatitis4 and uveitis.5 Many other diseases have been associated with HTLV-1, such as polymyositis,6 bronchial alveolar pneumonia,7 bronchiectasis,8 and Sjögren's syndrome,9–11 indicating multisystemic involvement in this infection. Moreover, other ocular lesions have also been associated with HTLV-1, such as corneal lesions,12 retinal vasculitis13 and Keratoconjunctivitis sicca (KCS).14–19 Although, the burden of HTLV-1 infection it is clearly demonstrated, this infection and its related diseases are still neglected.20
KCS, or dry eye disease (DED), is a multifactorial disease of the lacrimal film resulting in eye discomfort, visual disturbances, and tear film instability that could potentially damage the ocular surface.21 It is accompanied by increased osmolality of the tear film and inflammation of the ocular surface.22,23
The prevalence of KCS associated with HTLV-1 varies throughout the world. In Martinique, KCS prevalence was reportedly 37.0%15 vs. 15.4% in Japan.14 In Brazil, inconsistent prevalence has been reported: a study carried out in the state of São Paulo found a very low prevalence (3.9%),16 while others conducted in the states of Bahia and Minas Gerais reported between 27.5% to 36.4%.17,19 In addition, the number of studied patients also varied greatly, ranging from 52 to 262,15–17,19 and the clinical manifestations associated with KCS/HTLV-1 in these patients were poorly described. Moreover, studies evaluating the association between HTLV-1 proviral load and KCS are rare.18
Brazil, a country of more than 200 million inhabitants, represents one of the largest endemic areas for HTLV-1 and associated diseases in the world.24
Salvador, the capital of the State of Bahia, has the highest prevalence of HTLV-1 in the country.25,26 A population-based study estimated the prevalence of HTLV-1 at 1.7% in 2003, i.e. potentially 40,000 people could have been infected with HTLV-1 at that time.27
Therefore, the present study sought to determine the prevalence of HTLV-1-associated KCS using a substantially larger sample than the previous estimation, in addition to investigating clinical manifestations, virologic aspects and other associated factors, to more precisely estimate the magnitude of this health problem.
Subjects and methodsStudy design and populationAn outpatient cross-sectional study was conducted between June 2004 and September 2017 at the Integrative and Multidisciplinary Center for HTLV (CHTLV), Bahia School of Medicine and Public Health Salvador (EBMSP), Bahia-Brazil. Data from 1137 HTLV-1-infected patients was collected, including sociodemographic profile, date of HTLV serology and clinical status. All study volunteers provided written informed consent prior to inclusion in the present research protocol. For children informed consent were obtained from their parents or guardian. The Institutional Research Board of EBMSP approved this study (protocol no. 71/2006).
The study population comprised 1137 HTLV-1-infected individuals, of which 72.1% were females with age ranging from 4 to 93 years. The majority (38.4%) had less than eight years of education.
Laboratory, clinical and ophthalmologic evaluationHTLV-1 infection was diagnosed using several commercially available enzyme-linked immunosorbent (ELISA) (HTLV, enhanced, EIA, Cambridge Biotech Corporation, Worcester, MA) followed by Western Blot 2.4 (Genelabs Diagnostics GLD, Science Park Drive, Singapore) for confirmation and discrimination between HTLV-1 and HTLV-2. The quantification of the HTLV-1-proviral load was performed by RT-PCR TaqMan (Applied Biosystems) as previously described by the Dehee et al.28 Albumin DNA was used as an endogenous reference. Amplification and data acquisition were carried out using the ABI Prism 7700 Sequence detector system (Applied Biosystems). Standard curves were generated using a 10-fold serial dilution of a double-stranded plasmid (pcHTLV-ALB). The normalized value of the HTLV-1 proviral load was calculated as the ratio of (HTLV-1 DNA average copy number/albumin DNA average copy number)×2×106 and expressed as the number of HTLV-1×copies/106 cells. The clinical status of HTLV-1 patients with respect to HAM/TSP was determined according to the classification criteria established by De Castro-Costa et al.29
A complete ophthalmologic examination was performed in both eyes, including visual acuity as measured by the Snellen eye chart, in addition to optical correction, optical motility, applanation tonometry, biomicroscopy of the anterior and posterior chambers, and binocular indirect ophthalmoscopy. Lacrimal function was evaluated by break-up time (BUT), Rose Bengal and Schirmer I Tests. Tear BUT was performed via the instillation of 1% fluorescein solution (Fluorescein eye drops Ophtalmos®, São Paulo, Brazil), measuring the time required for dry spots to appear on the corneal surface after blinking. For Schirmer I testing, 5mm×35mm Whatman strips (Schirmer's tear test, Opthalmos®, São Paulo, Brazil) were placed in the lower fornix near the lateral canthus of both eyes for 5min. The Rose Bengal test was performed using 1% Rose Bengal staining solution (Rose Bengal eye drops; Ophthalmos®, São Paulo, Brazil), with results considered abnormal when a total Van-Bijsterveld score higher than three points was obtained. BUT scores <10s and <5mm for the Schirmer I test were considered abnormal.30 KCS diagnosis was considered in the presence of at least two out of three positive lacrimal function tests.31
All patients without the three lacrimal function tests required to diagnose KCS, and those presenting any previous palpebral disorders or nasolacrimal duct obstruction, as well as those who underwent intraocular surgery, were excluded. In addition, patients <18 years of age, a positive serology for Hepatitis B or C and HIV, diagnosis of Diabetes Mellitus,32 as well as the diagnosis of HAM/TSP possible and probable were excluded. In sum, only patients infected by HTLV-1, ≥18 years of age and those considered as definite HAM/TSP were included.
Data analysisStatistical analysis was performed using Stata software v. 13.0. Overall prevalence was calculated by dividing the number of KCS cases by the number of included patients assessed, expressed as a percentage. The presence of KCS was evaluated according to sociodemographic, clinical status, time of HTLV diagnosis and PVL using the Pearson chi-square test or Fisher's exact test, where appropriate. Crude and Adjusted Prevalence Rates (PR) with 95% Confidence Intervals (95% CI) were estimated using multivariate Poisson Regression with robust error variance. p values <0.05 were considered significant.
ResultsA total of 1137 HTLV-1 infected individuals were evaluated and 379 (33.4%) were excluded according to the following criteria: <18 years=17; incomplete ophthalmologic evaluations for KCS=207; positive serology for Hepatitis B or C=12 or HIV=3; HCV/HIV=1; diagnosis of diabetes=18; diagnosis of possible HAM/TSP=111, probable HAM/TSP=10. Accordingly, the resulting study sample included 758 individuals (1516 eyes).
A comparison between the excluded and included patients revealed differences with respect to age (48.5 [17.2] vs. 46.5 [14.2]; p=0.041, respectively) but not as regards sex (p=0.061). Furthermore, the number of individuals classified as definite HAM/TSP was greater in the excluded patients than in those enlisted (33.5% vs. 22.3%; p=0.001).
Ophthalmologic examinations revealed a diagnosis of KCS in 240 out of 758 patients, with a resulting overall prevalence of 31.7% (CI95%: 28.4–35.1). In contrast, the prevalence of KCS in patients with definite HAM-TSP was 49.1%.
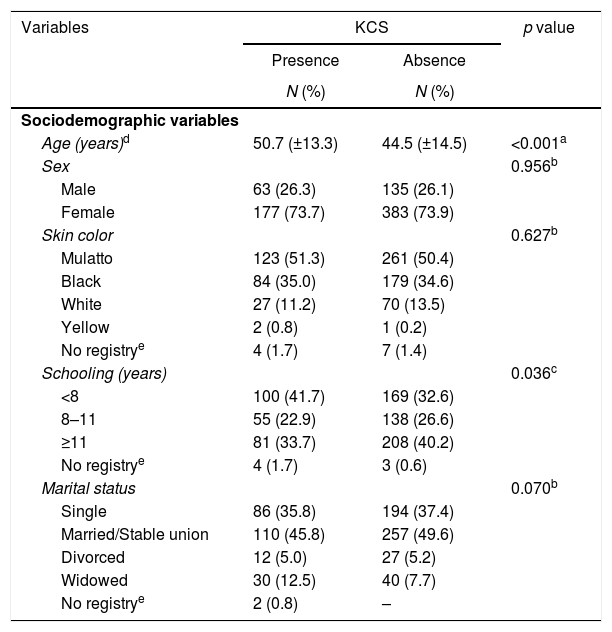
Table 1 comparatively lists the sociodemographic variables among KCS-positive patients and those without KCS. Concerning this sociodemographic data, while the KCS group was older (50.7 [13.3] vs. 44.5 [14.5] years; p<0.001) and more patients with KCS attended school for fewer than eight years (42.4% vs. 32.8%; p=0.04), no significant differences were detected with regard to sex, skin color or marital status.
Sociodemographic parameters of 758 Human T-Cell Lymphotropic Virus Type 1 infected patients.
| Variables | KCS | p value | |
|---|---|---|---|
| Presence | Absence | ||
| N (%) | N (%) | ||
| Sociodemographic variables | |||
| Age (years)d | 50.7 (±13.3) | 44.5 (±14.5) | <0.001a |
| Sex | 0.956b | ||
| Male | 63 (26.3) | 135 (26.1) | |
| Female | 177 (73.7) | 383 (73.9) | |
| Skin color | 0.627b | ||
| Mulatto | 123 (51.3) | 261 (50.4) | |
| Black | 84 (35.0) | 179 (34.6) | |
| White | 27 (11.2) | 70 (13.5) | |
| Yellow | 2 (0.8) | 1 (0.2) | |
| No registrye | 4 (1.7) | 7 (1.4) | |
| Schooling (years) | 0.036c | ||
| <8 | 100 (41.7) | 169 (32.6) | |
| 8–11 | 55 (22.9) | 138 (26.6) | |
| ≥11 | 81 (33.7) | 208 (40.2) | |
| No registrye | 4 (1.7) | 3 (0.6) | |
| Marital status | 0.070b | ||
| Single | 86 (35.8) | 194 (37.4) | |
| Married/Stable union | 110 (45.8) | 257 (49.6) | |
| Divorced | 12 (5.0) | 27 (5.2) | |
| Widowed | 30 (12.5) | 40 (7.7) | |
| No registrye | 2 (0.8) | – | |
KCS, Keratoconjunctivitis sicca.
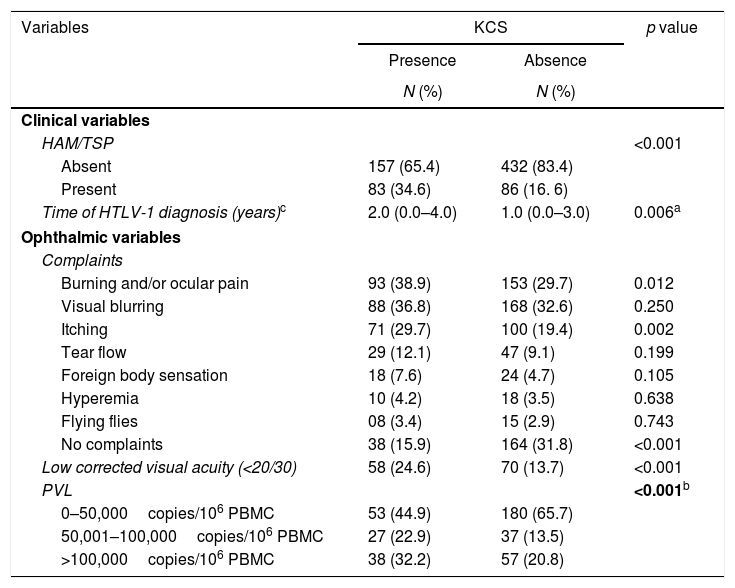
Table 2 comparatively lists the clinical and ophthalmological variables among the KCS-positive patients and those without KCS. More patients with KCS were classified as definite HAM/TSP (34.6% vs. 16.6%; p<0.001).
Clinical parameters and proviral load of 758 Human T-Cell Lymphotropic Virus Type 1 infected patients.
| Variables | KCS | p value | |
|---|---|---|---|
| Presence | Absence | ||
| N (%) | N (%) | ||
| Clinical variables | |||
| HAM/TSP | <0.001 | ||
| Absent | 157 (65.4) | 432 (83.4) | |
| Present | 83 (34.6) | 86 (16. 6) | |
| Time of HTLV-1 diagnosis (years)c | 2.0 (0.0–4.0) | 1.0 (0.0–3.0) | 0.006a |
| Ophthalmic variables | |||
| Complaints | |||
| Burning and/or ocular pain | 93 (38.9) | 153 (29.7) | 0.012 |
| Visual blurring | 88 (36.8) | 168 (32.6) | 0.250 |
| Itching | 71 (29.7) | 100 (19.4) | 0.002 |
| Tear flow | 29 (12.1) | 47 (9.1) | 0.199 |
| Foreign body sensation | 18 (7.6) | 24 (4.7) | 0.105 |
| Hyperemia | 10 (4.2) | 18 (3.5) | 0.638 |
| Flying flies | 08 (3.4) | 15 (2.9) | 0.743 |
| No complaints | 38 (15.9) | 164 (31.8) | <0.001 |
| Low corrected visual acuity (<20/30) | 58 (24.6) | 70 (13.7) | <0.001 |
| PVL | <0.001b | ||
| 0–50,000copies/106 PBMC | 53 (44.9) | 180 (65.7) | |
| 50,001–100,000copies/106 PBMC | 27 (22.9) | 37 (13.5) | |
| >100,000copies/106 PBMC | 38 (32.2) | 57 (20.8) | |
KCS, Keratoconjunctivitis sicca; HTLV-1, Human T-cell Lymphotropic Virus Type 1; HAM/TSP, HTLV-1-associated myelopathy/tropical spastic paraparesis; PVL, proviral load; PBMC, Peripheral Blood Mononuclear Cell.
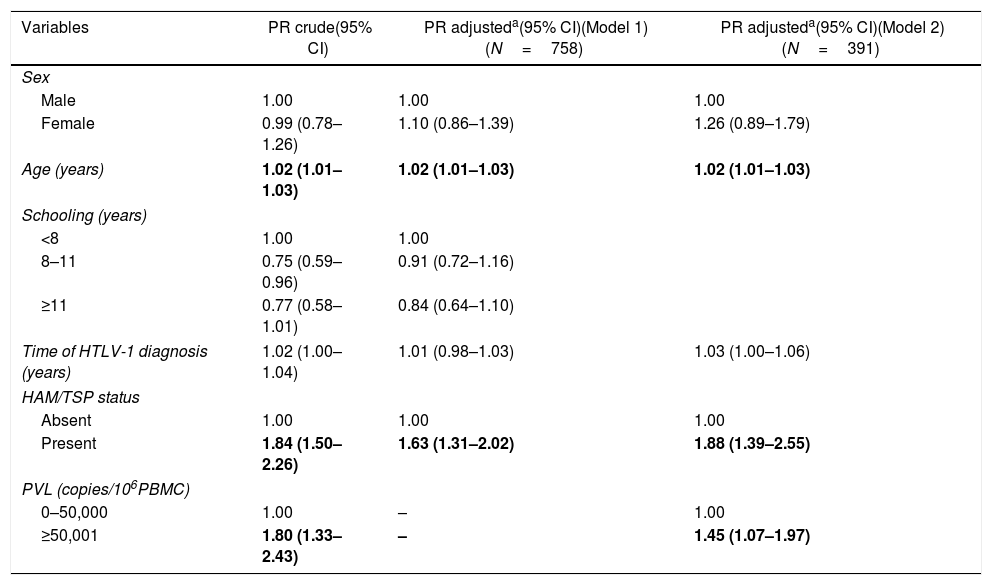
Table 3 details the crude and adjusted prevalence ratios of KCS in association with sociodemographic and clinical variables (model 1) and PVL (model 2). Model 1 demonstrated that age and the presence of HAM/TSP remained statistically significant, even after adjusting for sex, time of HTLV-1 diagnosis and duration of schooling. The prevalence of KCS was found to increase by 2%, on average, for every one-year increase in age. A diagnosis of definite HAM/TSP was associated with a 63% increase in the probability of developing KCS in comparison to those without HAM/TSP. Model 2, which included PVL, showed that levels of proviral load over 50,000copies/106 PBMC were associated with a 45% increase in the probability of developing KCS after adjusting for sex, age, time of HTLV-1 diagnosis and presence of HAM/TSP (Table 3). A comparison of proviral load between the excluded and included patients revealed no differences with respect to age (p=0.761), sex (p=0.817), presence of KCS (p=0.339) or time of diagnosis (p=0.243).
Crude and adjusted prevalence ratios (PRs), with respective 95% confidence intervals (95% CI), of association between presence of KCS and sociodemographic variables, time of diagnosis, HAM/TSP and PVL.
| Variables | PR crude(95% CI) | PR adjusteda(95% CI)(Model 1)(N=758) | PR adjusteda(95% CI)(Model 2)(N=391) |
|---|---|---|---|
| Sex | |||
| Male | 1.00 | 1.00 | 1.00 |
| Female | 0.99 (0.78–1.26) | 1.10 (0.86–1.39) | 1.26 (0.89–1.79) |
| Age (years) | 1.02 (1.01–1.03) | 1.02 (1.01–1.03) | 1.02 (1.01–1.03) |
| Schooling (years) | |||
| <8 | 1.00 | 1.00 | |
| 8–11 | 0.75 (0.59–0.96) | 0.91 (0.72–1.16) | |
| ≥11 | 0.77 (0.58–1.01) | 0.84 (0.64–1.10) | |
| Time of HTLV-1 diagnosis (years) | 1.02 (1.00–1.04) | 1.01 (0.98–1.03) | 1.03 (1.00–1.06) |
| HAM/TSP status | |||
| Absent | 1.00 | 1.00 | 1.00 |
| Present | 1.84 (1.50–2.26) | 1.63 (1.31–2.02) | 1.88 (1.39–2.55) |
| PVL (copies/106PBMC) | |||
| 0–50,000 | 1.00 | – | 1.00 |
| ≥50,001 | 1.80 (1.33–2.43) | – | 1.45 (1.07–1.97) |
KCS, Keratoconjunctivitis sicca; HTLV-1, Human T-cell Lymphotropic Virus Type 1; HAM/TSP, HTLV-1-associated myelopathy/tropical spastic paraparesis; PVL, proviral load; PBMC, Peripheral Blood Mononuclear Cell; PR, prevalence ratio.
Bold text indicate association with statistical significance.
Concerning the frequency of symptoms, burning and/or ocular pain (38.9% vs. 29.7%; p=0.012) and itching (29.7% vs. 19.4%; p=0.002) were significantly higher in the KCS group as compared to those without KCS. In addition, low corrected visual acuity on ophthalmologic examination was significantly higher (24.6%) vs. individuals without KCS (13.7%; p<0.001).
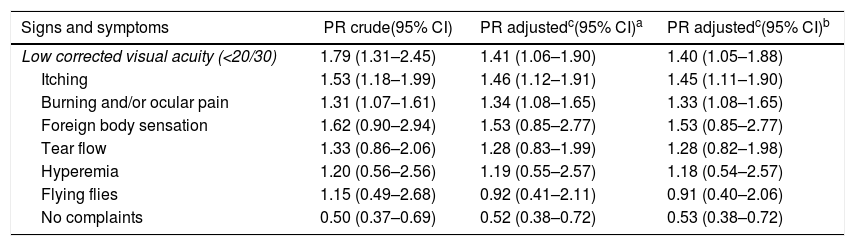
Table 4 describes the association between the presence of KCS and ophthalmic signs and symptoms. Even after adjusting for age and sex, patients with KCS presented a higher frequency of low acuity, burning and/or ocular pain and itching.
Crude and adjusted prevalence ratios of KCS in association with selected ophthalmic signs and symptoms.
| Signs and symptoms | PR crude(95% CI) | PR adjustedc(95% CI)a | PR adjustedc(95% CI)b |
|---|---|---|---|
| Low corrected visual acuity (<20/30) | 1.79 (1.31–2.45) | 1.41 (1.06–1.90) | 1.40 (1.05–1.88) |
| Itching | 1.53 (1.18–1.99) | 1.46 (1.12–1.91) | 1.45 (1.11–1.90) |
| Burning and/or ocular pain | 1.31 (1.07–1.61) | 1.34 (1.08–1.65) | 1.33 (1.08–1.65) |
| Foreign body sensation | 1.62 (0.90–2.94) | 1.53 (0.85–2.77) | 1.53 (0.85–2.77) |
| Tear flow | 1.33 (0.86–2.06) | 1.28 (0.83–1.99) | 1.28 (0.82–1.98) |
| Hyperemia | 1.20 (0.56–2.56) | 1.19 (0.55–2.57) | 1.18 (0.54–2.57) |
| Flying flies | 1.15 (0.49–2.68) | 0.92 (0.41–2.11) | 0.91 (0.40–2.06) |
| No complaints | 0.50 (0.37–0.69) | 0.52 (0.38–0.72) | 0.53 (0.38–0.72) |
KCS, Keratoconjunctivitis sicca; PR, Prevalence rate; CI, Confidence Intervals.
The present study represents an attempt to investigate the prevalence of KCS in association with HTLV-1 in a large cohort consisting of 758 patients. In addition, we present comprehensive clinical findings regarding significantly inferior corrected visual acuity, burning and/or pain, and itching in HTLV-1-positive patients with KCS. In addition, we confirmed a higher prevalence of KCS in definite HAM/TSP patients.
The overall prevalence of HTLV-1/KCS found in the present study was 31.7% (CI95%: 28.5–34.6), similar to estimates previously reported in two cities from Brazil, Salvador (36.4%; 39/107) in 200919 and Belo Horizonte (27.5%; 72/262 in 2006,17 as well as in Martinique (37%; 74/200) in 2002.15 These rates were much higher than the prevalence observed in asymptomatic carriers in São Paulo, Brazil (3.9%; 2/52).16 This discrepancy could be due to the absence of inclusion of individuals with HAM/TSP16 or to the criteria employed for diagnosing KCS. In contrast to Yamamoto et al., all other studies based a diagnosis of KCS on the presence of symptoms together with at least two out of three positive test results, namely BUT, Rose Bengal or Schirmer I. However, Yamamoto and colleagues diagnosed KCS exclusively on clinical findings consistent with dry eye, i.e. when abnormal results from all three tests were obtained, which could have led to an underestimation of the actual prevalence rate.33 In Japan, KCS is usually associated with Sjögren's syndrome, and the reported prevalence of HTLV-1 in patients with KCS was 15.4% in 1991.14,34 Unfortunately, due to the approach employed, these author's results were not suitable for inclusion in our comparison due to the reversed HTLV-1/KCS association.
The prevalence of KCS in patients with HAM/TSP (49.1%) found herein was sharply higher than in asymptomatic individuals, which is consistent with previous reports.15,17,19 Furthermore, we confirmed a positive association between KCS and HAM/TSP, which was approximately twice as common in individuals with definite HAM/TSP than in asymptomatic carriers, even after adjusting for age, sex, time of HTLV-1 diagnosis and schooling.15,17,19
Our study demonstrated that ocular burning and/or pain and itching were significantly more frequent in HTLV-1-patients with KCS, even after adjusting for sex and age. Moreover, the present data provide new evidence that HTLV-1/KCS patients had significantly lower corrected visual acuity compared to HTLV-1 individuals without KCS. The frequencies of clinical complaints, such as burning/pain, itching and inferior corrected visual acuity, were similar in individuals with KCS, regardless of HAM/TSP diagnosis (data not shown). In contrast to this finding, higher frequencies of burning and/or pain, as well as eye redness, have been described in HAM/TSP patients compared to both asymptomatic and uninfected individuals, while visual acuity and eye pressure were normal across all studied groups.17 In 2002, Merle et al. reported that the presence of ocular symptoms in HTLV-1-infected individuals is rare, and that ocular pruritus was the most commonly reported complaint.
However, due to the fact that the previous articles did not describe the frequencies of ophthalmological symptoms, a more robust comparison was not possible.
Based on epidemiological, clinical and experimental evidence, Sjögren's syndrome has been associated with KCS in association with HTLV-1 infection.9–11,34,35 This syndrome is an autoimmune disorder that evolves with lymphocytic infiltration in the exocrine glands, generally leading to xerostomia and/or KCS.36 However, the pathogenesis of HTLV-1-associated KCS might differ from what is observed in Sjögren's syndrome.34,37–39 Indeed, in a previous study conducted in patients with KCS diagnosis from the CHTLV cohort, no patients tested positive for ANA, anti-SSA/Ro, anti-SSB/La or RF autoantibodies,38 which was similar to previous reports.11,15,37 Thus, the mechanism underlying HTLV-1-associated KCS could be either directly or indirectly related to the virus itself.34 Herein, we confirmed that patients with KCS had significantly higher HTLV-1 proviral load than patients without the disease, regardless the presence of HAM/TSP.18 Indeed, in the present study, evaluating a large sample we demonstrated that HTLV-1 proviral load >500,000copies/106 PBMC was shown to be significantly associated with KCS. Also, higher production of proinflammatory cytokines (IFN-γ and TNF-α) were found in HTLV-1 infected patients with KCS than in HTLV-1 infected subjects without dry eye syndrome, indicating that an exacerbated proinflammatory response may play a role in the destruction of the salivary and lacrimal glands observed during HTLV-1 infection.39
While the absence of an uninfected control group was a relevant limitation, previous controlled studies carried out in the Brazilian state of Minas Gerais and Martinique15,17 reported a significantly higher prevalence of KCS in HTLV-1-infected patients than in uninfected individuals. In addition, the patients who were excluded herein were older and had a higher proportion of HAM/TSP. These aspects may have reduced the magnitude of the strength of association between HAM/TSP and KCS. Despite the loss of 366 dosages of PVL (48.3%), a comparison between the excluded and included patients revealed no differences with respect to age, sex, presence of KCS and time of diagnosis.
Of note, burning/pain, itching and low corrected visual acuity, the most common symptoms of KCS found herein, could interfere greatly in patient quality of life.40 Therefore, early diagnosis of KCS allows for preventive and therapeutic measures to avoid chronic clinical changes on the ocular surface, including palpebral and corneal disorders, such as keratitis, neovascularization, opacification and predisposition to ulcer formation.21,41,42 Treatment options for KCS include treatments for lacrimal insufficiency and eyelid abnormalities, as well as anti-inflammatory drugs, surgical approaches, dietary modifications, environmental modifications, as well as complementary therapies. Finally, based on the results obtained herein, it is strongly recommended that HTLV-I patients undergo periodic ophthalmologic examination.
Conflicts of interestThe authors declare no conflicts of interest.
We thank the Conselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq) (301092/2018-4), Fundação de Amparo à Pesquisa do Estado da Bahia (Fapesb) (CNV0072/2013) and Fundação Nacional para o Desenvolvimento do Ensino Superior (Funadesp) for financial support, Mr. Noilson Lazaro Gonçalves for technical assistance, Ms. Sonia Rangel for help in reviewing medical records, and Andris K. Walter for providing English language revision and manuscript copyediting assistance.