Influenza burden in Brazil is considerable with 4.2–6.4 million cases in 2008 and influenza-like-illness responsible for 16.9% of hospitalizations. Cost-effectiveness of influenza vaccination may be assessed by different types of models, with limitations due to data availability, assumptions, and modelling approach.
ObjectiveTo understand the impact of model complexity, the cost-utility of quadrivalent versus trivalent influenza vaccines in Brazil was estimated using three distinct models: a 1-year decision tree population model with three age groups (FLOU); a more detailed 1-year population model with five age groups (FLORA); and a more complex lifetime multi-cohort Markov model with nine age groups (FLORENCE).
MethodsAnalysis 1 (impact of model structure) compared each model using the same data inputs (i.e., best available data for FLOU). Analysis 2 (impact of increasing granularity) compared each model populated with the best available data for that model.
ResultsUsing the best data for each model, the discounted cost-utility ratio of quadrivalent versus trivalent influenza vaccine was R$20,428 with FLOU, R$22,768 with FLORA (versus R$20,428 in Analysis 1), and, R$19,257 with FLORENCE (versus R$22,490 in Analysis 1) using a lifetime horizon. Conceptual differences between FLORA and FLORENCE meant the same assumption regarding increased all-cause mortality in at-risk individuals had an opposite effect on the incremental cost-effectiveness ratio in Analysis 2 versus 1, and a proportionally higher number of vaccinated elderly in FLORENCE reduced this ratio in Analysis 2.
DiscussionFLOU provided adequate cost-effectiveness estimates with data in broad age groups. FLORA increased insights (e.g., in healthy versus at-risk, paediatric, respiratory/non-respiratory complications). FLORENCE provided greater insights and precision (e.g., in elderly, costs and complications, lifetime cost-effectiveness).
ConclusionAll three models predicted a cost per quality-adjusted life year gained for quadrivalent versus trivalent influenza vaccine in the range of R$19,257 (FLORENCE) to R$22,768 (FLORA) with the best available data in Brazil (Appendix A).
The annual number of confirmed influenza cases in Brazil was estimated to be between 4.2 and 6.4 million cases in 2008.1 While data were limited due to likely underreporting, the influenza surveillance system reported that influenza-like illness was responsible for 4.4–16.9% of hospital consultations between 2000 and 2008.2 Data on mortality were reported for influenza and pneumonia combined, and were highest among the youngest and eldest age groups in most Latin American countries. The highest proportion of deaths in children under five years in the region were reported for Ecuador (14.4% in 2003) and Brazil (13.5% in 2004).1 The vaccination target group in Brazil has become progressively broader since 1999, and now includes people over 60 years old, children aged six months to four years, and a range of vulnerable people.2
By investing in disease prevention, influenza vaccination programs can increase the health of the entire population. Policy-makers need to choose which age- and risk-groups to vaccinate in order to achieve the best health outcomes. Investment costs need to be weighed up against the current health burden, expected health gains, and cost savings, to evaluate whether vaccination programs offer value for money compared to existing disease management options. Epidemiologic and economic models, combining current knowledge of the disease burden, transmission and impact on healthcare resources are frequently used to predict the health and economic consequences of vaccination. A range of model types are available with many different data requirements; more detailed approaches typically require more data, which can often be unavailable leading to increased use of assumptions, and ultimately reducing validity of a more complex approach.
Regarding the cost-effectiveness of influenza vaccination, a range of model types have been used, but with caveats relating to limitations in the modelling approach, lack of input data, and use of assumptions. Health policy guidelines recommend annual influenza vaccination in consecutive seasons, yet many influenza models consider cost-effectiveness in one year and apply a lifetime horizon to assess quality-adjusted life-years (QALYs) lost due to premature mortality.3–5 These 1-year models may artificially oversimplify lifetime effects by assuming all influenza mortality occurs at one average age within an age group, and those who survive influenza would live their remaining life expectancy at a constant baseline utility. The population of these 1-year models is often broadly subdivided (e.g. children, adults, and elderly), however, there is considerable heterogeneity within those broad age bands, especially among the elderly (e.g., due to natural mortality, baseline utility and costs). Multi-cohort models in which cohorts enter the model at many different ages and are followed over a lifetime of consecutive influenza seasons, provide a more direct approach to influenza management than 1-year models, consider heterogeneity in the population, and allow for an appropriate attribution of QALYs over time.6 However, detailed age-specific data may prove difficult to find.
This paper aims to understand the impact model complexity has on predicting results, and the pros and cons of different approaches. In order to do so, the impact of introducing influenza vaccination in Brazil was estimated using three distinct models, from a 1-year decision tree population model (FLOU) to a more complex life-time multi-cohort Markov model (FLORENCE), and with a moderately complex 1-year population model (FLORA). Thus FLOU, FLORA, and FLORENCE, each used increasing data and modelling complexity, were compared in terms of predicting outcomes with increasing precision. The models compared cases, costs and health outcomes of the following influenza vaccination strategies in Brazil: no vaccination, trivalent influenza vaccination (TIV), and quadrivalent influenza vaccination (QIV).
MethodsModel descriptionsFLOU (i.e. inFLuenza cOst-Utility) modelThe FLOU model is a decision tree population model dividing the population into three age groups (paediatric, adult, and elderly; <18, 18–64, and ≥65 years, respectively), each subdivided into two risk groups (healthy and at-risk). The model uses a 1-year time horizon, while attributing lifetime QALY losses to premature deaths. Influenza cases could lead to general practitioner (GP) visits, hospitalization, and death following hospitalization or no hospitalization.
A distinction was made between healthy and at-risk populations for vaccination coverage, and the probability of GP visits and hospitalization. The model calculated vaccination costs (vaccine price and administration), GP visit and hospitalization costs as well as baseline utilities, QALY loss due to influenza, hospitalizations, and mortality for each strategy.
To avoid oversimplification of lifetime benefit calculations observed in other 1-year models, a life table approach was implemented to estimate (quality-adjusted) life expectancy ((QA)LE) at age of premature death; age-dependent baseline utilities, probabilities of all-cause mortality, and discounting were included, with a defined discount rate for outcomes. Finally, the weighted average of (QA)LE was estimated for each age group.
FLORA modelTo increase the sensitivity of the analysis, another 1-year decision tree population model called FLORA was developed, with more granularity than FLOU. Influenza could lead to GP visits, antiviral treatment with or without resistance in at-risk populations, respiratory or non-respiratory complications leading to outpatient treatment or hospitalization, and influenza death with or without prior complications. The FLORA model structure included five age-groups (i.e., <7 months, 7–24 months, 3–17 years, 18–64 years, 65+ years). Additional parameters compared to FLOU allowed for further differentiation between healthy and at-risk populations (e.g., probabilities of influenza, probabilities of complications (respiratory and non-respiratory), death following hospitalization, outpatient treatment, no complication, and QALY loss per premature death). The societal perspective considered direct and indirect medical costs. Disutilities associated with influenza complications treated in an outpatient setting were also included.
The calculation of (QA)LE was adapted to account for typically lower baseline utilities and the higher risk of natural mortality in at-risk individuals, and thus a shorter life expectancy in this risk-group. In addition, the life table approach allowed for a proportion of healthy people to become at-risk with age, to maintain the actual population distribution over time/age despite the higher mortality in the at-risk population. More accurate estimates of life expectancy in the healthy population were thus obtained.
The decision tree model structures of FLOU (Fig. A1) and FLORA (Fig. A2) are presented in Appendix B.
FLORENCE (i.e. InFLuenza cOmpREhENsive Cost-Effectiveness) modelThe FLORENCE model is a multi-cohort Markov model with nine age groups (including five age groups for the elderly) followed over a lifetime horizon with consecutive influenza seasons in annual model cycles. The model was previously used to assess influenza vaccination in the UK.6 In comparison to FLORA, FLORENCE added more granularity in model structure (e.g., post-exposure prophylaxis (PEP), emergency room (ER) visits for influenza, three respiratory complications and five non-respiratory complications) and in data inputs (e.g., probabilities, costs and/or health outcomes) related to vaccination adverse events, PEP, antibiotics, nursing home visits, herd immunity (static approach) and more societal costs (e.g., non-reimbursed medical costs and non-medical costs).
Vaccination was applied in each annual cycle, and cumulative QALYs lost due to influenza mortality were directly calculated via the cohort approach. Hence, unlike in FLOU and FLORA, age-dependent life expectancy estimates were not required as proxies for QALYs lost due to influenza mortality.
Model analysesTwo analyses were conducted: the first to assess the impact of changing model structure on results, and the second to assess the impact of increasing granularity in inputs and outputs.
Analysis 1 estimated the impact of model structure and compared outcomes when the same data inputs and settings were used for all three models. The FLOU model was populated with the best available data for Brazilian children, adults, and elderly, and FLORA and FLORENCE were populated with the same FLOU data inputs (e.g., if 12.8% of the paediatric group were at-risk of clinical influenza in FLOU, then 12.8% was used for all age groups <18 years in FLORA and FLORENCE). Only the population distribution across age groups differed between models, calculated as the population size of the age-group divided by the total population in Brazil. Since data inputs were the same across the models, any observed differences would be attributable to the model structure.
Analysis 2 estimated the impact of increasing the level of granularity (e.g., assessing heterogeneity in the population) and compared outcomes from each model being populated with the best available data for Brazil according to their specific data requirements. In the first instance, outcomes in the arm with no vaccination were compared across models. Identical cases and costs were expected with FLOU and FLORA and, when considering a 1-year time horizon, in FLORENCE. Then, the results with vaccination were compared, with differences reflecting the increased precision of data inputs.
Setting, perspective, discount rate, currency and price dateThe public healthcare payer perspective in Brazil was used in FLORA and FLORENCE to allow comparisons with FLOU which did not include the societal perspective. Similarly, the analysis with FLORENCE excluded costs and effects due to PEP, vaccination adverse events, nursing home visits and herd immunity, to allow comparisons to FLOU and FLORA outputs.
All costs (2015 Brazilian Real, R$) and health outcomes were discounted at 5%. Costs were based on the Brazilian Unified Health System (Sistema Unico de Saude, SUS) which applies the same reimbursement costs to all regions of the country. Discounting had no impact on costs in the FLOU and FLORA models given their 1-year time horizon, but did have an impact on health outcomes, as lifetime QALYs lost were calculated for premature deaths. In the FLORENCE model, future costs (avoided) were discounted in the year in which they occurred and annually recurrent costs associated with one influenza case (e.g. long-term sequelae) were not included. Regarding mortality, (QA)LYs lost were discounted every year of the time horizon of the model. Discounting therefore had a greater impact on health outcomes than on costs.
Outcomes assessedThe epidemiologic outcomes assessed were: number vaccinated, influenza cases, GP visits (and ER visits in FLORENCE) for uncomplicated influenza, influenza complications with hospital or outpatient treatment (the latter only for FLORA and FLORENCE), and influenza deaths with or without prior complications. The economic outcomes assessed were vaccination costs (vaccine price and administration), neuraminidase inhibitors (NI) treatment costs (i.e. NI drugs and antibiotics, only for FLORA and FLORENCE), GP visit costs (ER costs, only for FLORENCE), influenza complication treatment costs (hospital or outpatient treatment, the latter only for FLORA and FLORENCE). The health outcomes measured were life-years gained during time horizon and life-years lost due to premature mortality, QALYs gained, using baseline utilities and utility decrements due to influenza, hospital or outpatient treatment for complications (the latter only for FLORA and FLORENCE), and premature mortality. Differences in health outcomes and costs between the QIV and TIV arms were compared in terms of incremental cost per LY gained and per QALY gained.
When comparing outcomes using a 1-year time horizon, the accumulated (QA)LYs gained in the FLORENCE model did not reflect the impact of premature mortality because the FLORENCE model is a multi-cohort lifetime model where LYs and QALYs are accumulated over time. No results could thus be produced in terms of health outcomes associated with influenza mortality with the FLORENCE 1-year time horizon. This means that the lifetime (QA)LYs lost due to mortality could not be considered with a 1-year time horizon. However, the baseline utilities gained and QALYs lost due to influenza and hospitalization could be extracted and compared to the 1-year FLOU and FLORA models.
Model inputs for Analyses 1 and 2Appendix C presents the input tables used in Analysis 2 (=best available data by model). The data inputs used for Analysis 1 in the three models are the FLOU data inputs of Appendix C. Appendix D presents the assumptions and source data used for the calculation of the data inputs (i.e., demographics, vaccine inputs, resource use, complications and hospitalization, costs, and utilities).
During data input calculations, two important adjustments were taken into consideration with regard to collecting/calculating data inputs for age-groups covering different age boundaries, as was the case in the FLOU, FLORA, and FLORENCE models.
Firstly, a commonly used approach to obtaining a weighted average for a modelled age group covering multiple age groups of the population in the source reference was to use the crude population distribution of the model to calculate the proportional age-distribution. This is correct as long as the crude population distribution in the model is exactly the same as the modelled age distribution of the parameter investigated. For instance, to calculate the probability that a complication is a respiratory complication in healthy individuals, the proportional age-distribution should consider not only the crude population distribution but also the probability of being healthy, the probability of influenza, and the probability of influenza complications in healthy individuals. It was therefore important that weighted average calculations considered the correct proportional age-distribution of the population considered in the source reference, e.g. the age-distribution of respiratory complications can be substantially different from the age distribution of the total population.
Secondly, reported pooled results in publications rarely matched the modelled population. Age-stratified data were selected above pooled data. For instance, when data was available for a full age-group (i.e., children) as well as for subgroups (i.e., 0–5, 6–12 and 13–17 years), the calculations were performed on the subgroups instead of the pooled data. Using the latter implies that the population distribution of the publication matches the modelled population distribution, which is not the case.
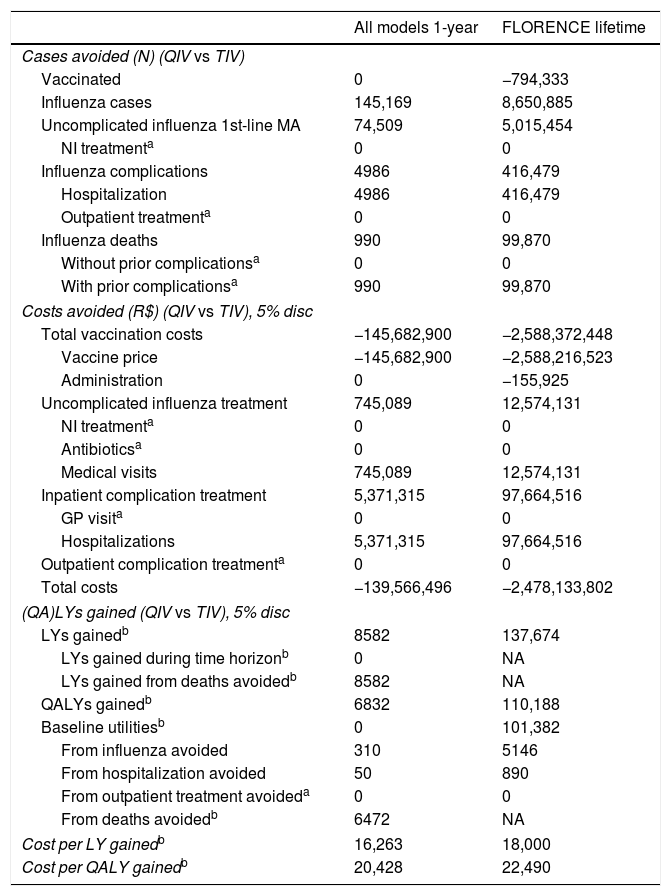
ResultsAnalysis 1: impact of model structure on vaccination outcomes with identical data inputs for all three modelsTable 1 presents the cases and costs avoided with a 1-year time horizon for QIV versus TIV with all three models in a single column, as these results were identical across the models. In a separate column, FLORENCE lifetime results (for QIV versus TIV) are reported. Disaggregated results in terms of cases, costs, and QALYs with TIV and QIV are presented in Appendix E.
Difference in cases and discounted costs, QALYs and cost-utility ratio with QIV versus TIV for all three models using FLOU inputs for Brazil.
| All models 1-year | FLORENCE lifetime | |
|---|---|---|
| Cases avoided (N) (QIV vs TIV) | ||
| Vaccinated | 0 | −794,333 |
| Influenza cases | 145,169 | 8,650,885 |
| Uncomplicated influenza 1st-line MA | 74,509 | 5,015,454 |
| NI treatmenta | 0 | 0 |
| Influenza complications | 4986 | 416,479 |
| Hospitalization | 4986 | 416,479 |
| Outpatient treatmenta | 0 | 0 |
| Influenza deaths | 990 | 99,870 |
| Without prior complicationsa | 0 | 0 |
| With prior complicationsa | 990 | 99,870 |
| Costs avoided (R$) (QIV vs TIV), 5% disc | ||
| Total vaccination costs | −145,682,900 | −2,588,372,448 |
| Vaccine price | −145,682,900 | −2,588,216,523 |
| Administration | 0 | −155,925 |
| Uncomplicated influenza treatment | 745,089 | 12,574,131 |
| NI treatmenta | 0 | 0 |
| Antibioticsa | 0 | 0 |
| Medical visits | 745,089 | 12,574,131 |
| Inpatient complication treatment | 5,371,315 | 97,664,516 |
| GP visita | 0 | 0 |
| Hospitalizations | 5,371,315 | 97,664,516 |
| Outpatient complication treatmenta | 0 | 0 |
| Total costs | −139,566,496 | −2,478,133,802 |
| (QA)LYs gained (QIV vs TIV), 5% disc | ||
| LYs gainedb | 8582 | 137,674 |
| LYs gained during time horizonb | 0 | NA |
| LYs gained from deaths avoidedb | 8582 | NA |
| QALYs gainedb | 6832 | 110,188 |
| Baseline utilitiesb | 0 | 101,382 |
| From influenza avoided | 310 | 5146 |
| From hospitalization avoided | 50 | 890 |
| From outpatient treatment avoideda | 0 | 0 |
| From deaths avoidedb | 6472 | NA |
| Cost per LY gainedb | 16,263 | 18,000 |
| Cost per QALY gainedb | 20,428 | 22,490 |
QIV vs TIV, quadrivalent versus trivalent influenza vaccine; MA, medical advice; NI, neuraminidase inhibitors; GP, general practitioner; LY, life-year; QALY, quality-adjusted life-year; NA, not applicable; disc, discounted.
All three models used the same inputs (from FLOU). The results showed an identical number of cases and costs in all three models with a 1-year horizon. Overall, QIV prevented more influenza cases, complications and deaths than TIV, resulting in fewer GP and hospitalization costs. Despite saving disease management costs, vaccination costs with QIV were higher than TIV due to the higher price of QIV vaccine. In FLORENCE with a lifetime horizon, QIV resulted in fewer influenza cases and associated deaths, resulting in higher survival and therefore more individuals to be vaccinated. The (QA)LYs gained with FLOU and FLORA were identical, and matched the QALYs due to influenza, outpatient treatment, and hospitalization which could be extracted from the FLORENCE 1-year model. Overall, QIV resulted in more QALYs gained than TIV from preventing influenza cases, complications and deaths.
The discounted cost per LY gained with QIV versus TIV was R$16,263 with the FLOU/FLORA 1-year models, and R$18,000 with FLORENCE using a lifetime horizon. The discounted cost-utility ratio was R$20,428 per QALY gained with FLOU/FLORA 1-year models, and R$22,490 with FLORENCE using a lifetime horizon. Given that FLOU and FLORA used one broad age group to represent the elderly, all subjects accrued the same number of LYs lost per premature death (i.e., 8.22 years). In FLORENCE with five elderly age groups, subjects died on average at an older age and thus had fewer LYs lost due to premature death, resulting in a lower (QA)LY gain due to mortality and the higher cost per (QA)LY observed. This effect was reinforced by higher survival with QIV, resulting in more persons being vaccinated at later ages, and with fewer LYs lost due to premature death.
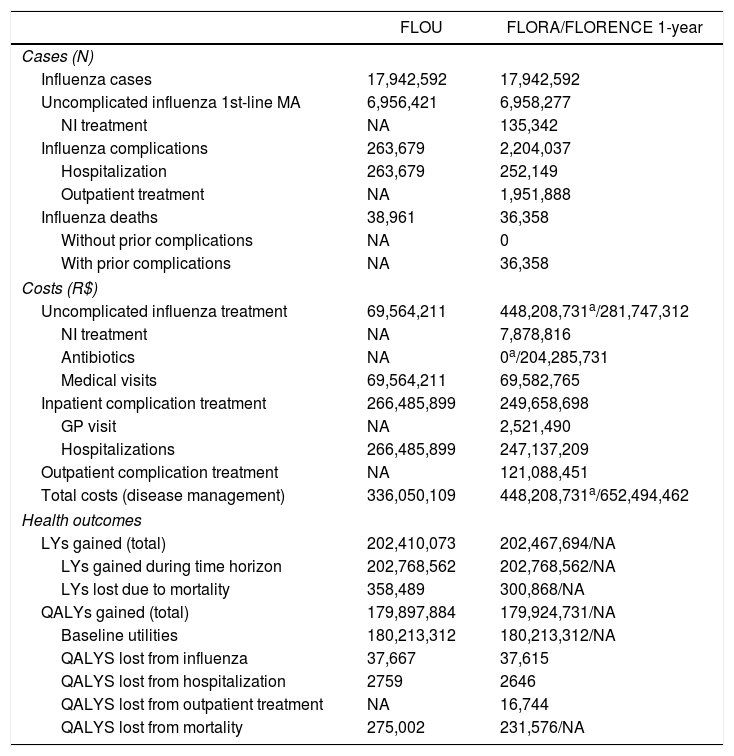
Analysis 2: impact of increased granularity on model outcomes with all three models populated with best available dataAnalysis of the no vaccination arms in the 1-year models populated with best available dataThe ‘no vaccination’ arms of the FLOU, FLORA and FLORENCE 1-year models populated with the best available data for Brazil were compared in terms of cases, costs, and outcomes (Table 2). Overall, results differed with FLOU compared to FLORA and FLORENCE, due to FLOU's model structure with fewer age-groups.
Cases, costs and health outcomes with no vaccination in the 1-year models populated with best available data inputs.
| FLOU | FLORA/FLORENCE 1-year | |
|---|---|---|
| Cases (N) | ||
| Influenza cases | 17,942,592 | 17,942,592 |
| Uncomplicated influenza 1st-line MA | 6,956,421 | 6,958,277 |
| NI treatment | NA | 135,342 |
| Influenza complications | 263,679 | 2,204,037 |
| Hospitalization | 263,679 | 252,149 |
| Outpatient treatment | NA | 1,951,888 |
| Influenza deaths | 38,961 | 36,358 |
| Without prior complications | NA | 0 |
| With prior complications | NA | 36,358 |
| Costs (R$) | ||
| Uncomplicated influenza treatment | 69,564,211 | 448,208,731a/281,747,312 |
| NI treatment | NA | 7,878,816 |
| Antibiotics | NA | 0a/204,285,731 |
| Medical visits | 69,564,211 | 69,582,765 |
| Inpatient complication treatment | 266,485,899 | 249,658,698 |
| GP visit | NA | 2,521,490 |
| Hospitalizations | 266,485,899 | 247,137,209 |
| Outpatient complication treatment | NA | 121,088,451 |
| Total costs (disease management) | 336,050,109 | 448,208,731a/652,494,462 |
| Health outcomes | ||
| LYs gained (total) | 202,410,073 | 202,467,694/NA |
| LYs gained during time horizon | 202,768,562 | 202,768,562/NA |
| LYs lost due to mortality | 358,489 | 300,868/NA |
| QALYs gained (total) | 179,897,884 | 179,924,731/NA |
| Baseline utilities | 180,213,312 | 180,213,312/NA |
| QALYS lost from influenza | 37,667 | 37,615 |
| QALYS lost from hospitalization | 2759 | 2646 |
| QALYS lost from outpatient treatment | NA | 16,744 |
| QALYS lost from mortality | 275,002 | 231,576/NA |
NI, neuraminidase inhibitors; GP, general practitioner; LY, life-year; QALY, quality-adjusted life-year; NA, not applicable.
All three models predicted the same number of influenza cases in one year. However, FLOU had fewer cases seeking first line medical advice (MA). This difference is attributable to the different data inputs in FLOU versus FLORA for the probability of influenza. FLORA distinguished between the probability of influenza in healthy and at-risk individuals. A weighted average probability for each group was calculated based on their respective proportional age-distribution, obtained by multiplying the corresponding population age-distribution with the healthy/at-risk distribution. In FLOU, the proportional age-distribution only considered the population distribution (since no distinction was made between the probability of influenza in healthy and at-risk individuals).
FLOU had a higher number of hospitalizations and deaths compared to FLORA and FLORENCE, since FLORA and FLORENCE included the use of NI treatment for at-risk individuals reducing the risk of developing influenza-related complications.
The cost differences between the models reflected the different number of cases, i.e., lower costs for outpatient treatment of uncomplicated influenza and higher hospitalization costs for FLOU. FLORENCE conveyed higher costs than FLORA due to the inclusion of antibiotics and associated costs.
There were more LYs and QALYs lost due to mortality in FLOU compared with FLORA due to the distinction between healthy and at-risk individuals, with fewer QALYs lost in the case of premature death in at-risk individuals compared to healthy individuals. Since at-risk individuals had a higher probability of influenza death, they were overrepresented (compared to the population distribution) in the average influenza deaths, in turn leading to fewer (QA)LYs lost due to influenza mortality in FLORA versus FLOU. Fewer QALYs were lost due to influenza in FLORA and FLORENCE compared with FLOU, as NI treatment reduced the duration of influenza and therefore the QALY loss. Where 1-year data could be calculated from the FLORENCE model, these were identical to FLORA (e.g., QALY loss due to influenza, hospitalization and outpatient treatment) (Table 2).
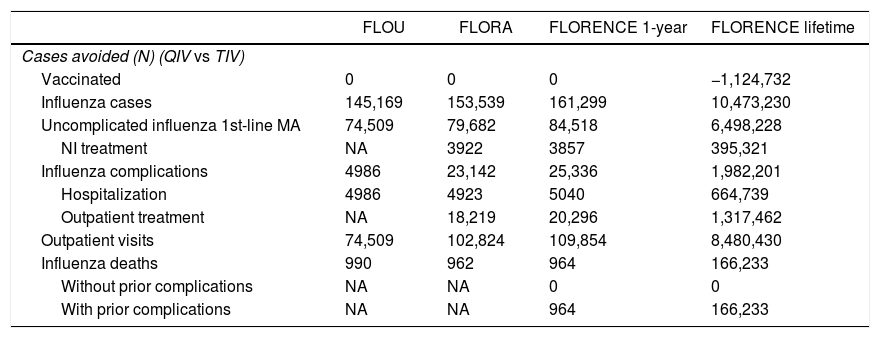
Analysis of the vaccination arms populated with best available dataIn this analysis, the best data available for Brazil in each model was used to compare vaccination with QIV versus TIV. Disaggregated results in terms of cases, costs, and QALYs with TIV and QIV are presented in Appendix F, and QIV versus TIV outcomes are presented in Table 3.
Cases avoided with QIV vs TIV in the models populated with best available data inputs.
| FLOU | FLORA | FLORENCE 1-year | FLORENCE lifetime | |
|---|---|---|---|---|
| Cases avoided (N) (QIV vs TIV) | ||||
| Vaccinated | 0 | 0 | 0 | −1,124,732 |
| Influenza cases | 145,169 | 153,539 | 161,299 | 10,473,230 |
| Uncomplicated influenza 1st-line MA | 74,509 | 79,682 | 84,518 | 6,498,228 |
| NI treatment | NA | 3922 | 3857 | 395,321 |
| Influenza complications | 4986 | 23,142 | 25,336 | 1,982,201 |
| Hospitalization | 4986 | 4923 | 5040 | 664,739 |
| Outpatient treatment | NA | 18,219 | 20,296 | 1,317,462 |
| Outpatient visits | 74,509 | 102,824 | 109,854 | 8,480,430 |
| Influenza deaths | 990 | 962 | 964 | 166,233 |
| Without prior complications | NA | NA | 0 | 0 |
| With prior complications | NA | NA | 964 | 166,233 |
QIV vs TIV, quadrivalent versus trivalent influenza vaccine; MA, medical advice; NI, neuraminidase inhibitors; NA, not applicable.
In all three models, QIV prevented more influenza cases and deaths, and reduced resource utilization (e.g., in/outpatient visits and treatment of un/complicated influenza) compared with TIV. When comparing the models within a 1-year time horizon, the best outcomes for QIV were mainly achieved in the FLORENCE model; i.e., most influenza cases prevented, most visits prevented in GP, hospital and outpatient settings. The number of NI treatments prevented was higher with FLORA. NI treatment was only provided to at-risk individuals seeking MA. There were fewer influenza cases avoided with QIV in at-risk individuals in FLORENCE (despite a higher total number of influenza cases avoided) and thus less NI treatments could be avoided compared with FLORA.
Given that the influenza cases in the ‘no vaccination’ arm of FLORA and FLORENCE 1-year models were identical (Table 2), differences in numbers of influenza cases in the ‘vaccination’ arms were due to vaccination coverage and vaccine efficacies (VE). Slightly more hospitalizations and deaths are avoided in the FLOU model compared to FLORA and FLORENCE 1-year. This is because NI treatment is not considered in the FLOU model and hence there is no associated reduction in risk of complications. Therefore, the impact of vaccination on complications and further consequences thereof will be higher in FLOU.
As was the case in Analysis 1, the FLORENCE lifetime horizon analysis found more individuals vaccinated with QIV than TIV, due to better survival in the QIV arm which resulted in more people eligible for vaccination.
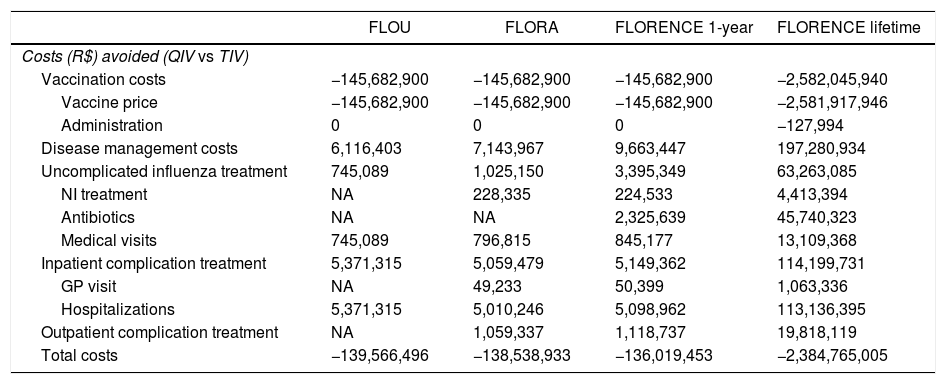
Vaccination costs were identical across models and higher with QIV versus TIV (Appendix F). Overall, the highest disease management cost savings with QIV versus TIV were shown in the FLORENCE 1-year model, mainly due to cost savings in antibiotics and outpatient complication treatment (included in this model's structure and inputs) (Table 4).
Costs avoided with QIV versus TIV in the models populated with best available data inputs.
| FLOU | FLORA | FLORENCE 1-year | FLORENCE lifetime | |
|---|---|---|---|---|
| Costs (R$) avoided (QIV vs TIV) | ||||
| Vaccination costs | −145,682,900 | −145,682,900 | −145,682,900 | −2,582,045,940 |
| Vaccine price | −145,682,900 | −145,682,900 | −145,682,900 | −2,581,917,946 |
| Administration | 0 | 0 | 0 | −127,994 |
| Disease management costs | 6,116,403 | 7,143,967 | 9,663,447 | 197,280,934 |
| Uncomplicated influenza treatment | 745,089 | 1,025,150 | 3,395,349 | 63,263,085 |
| NI treatment | NA | 228,335 | 224,533 | 4,413,394 |
| Antibiotics | NA | NA | 2,325,639 | 45,740,323 |
| Medical visits | 745,089 | 796,815 | 845,177 | 13,109,368 |
| Inpatient complication treatment | 5,371,315 | 5,059,479 | 5,149,362 | 114,199,731 |
| GP visit | NA | 49,233 | 50,399 | 1,063,336 |
| Hospitalizations | 5,371,315 | 5,010,246 | 5,098,962 | 113,136,395 |
| Outpatient complication treatment | NA | 1,059,337 | 1,118,737 | 19,818,119 |
| Total costs | −139,566,496 | −138,538,933 | −136,019,453 | −2,384,765,005 |
Negative values=incremental costs, positive values=cost savings.
QIV vs TIV, quadrivalent versus trivalent influenza vaccine; NI, neuraminidase inhibitors; GP, general practitioner; NA, not applicable.
Compared to FLORA, there were more LYs and QALYs lost due to mortality with TIV and QIV in FLOU, as the latter predicted more deaths and made no distinction between healthy and at-risk individuals’ life expectancy. Influenza mortality was the key driver of health outcomes. The QALYs lost with TIV and QIV due to influenza and hospitalization were also higher in FLOU vs FLORA reflecting the higher number of cases. In FLORA compared to FLORENCE 1-year model, there were more QALYs lost due to influenza, hospitalizations, and outpatient treatment with QIV and TIV reflecting the higher number of cases (Appendix F).
The LYs and QALYs gained with QIV versus TIV were higher in FLOU versus FLORA because of more deaths are avoided in FLOU and because the FLORA model included a lower average (QA)LE per premature death in at-risk individuals. The FLORENCE 1-year model, however, gained most QALYs due to influenza, hospitalization, and outpatient treatment, due to higher numbers of cases avoided with QIV (Table 5).
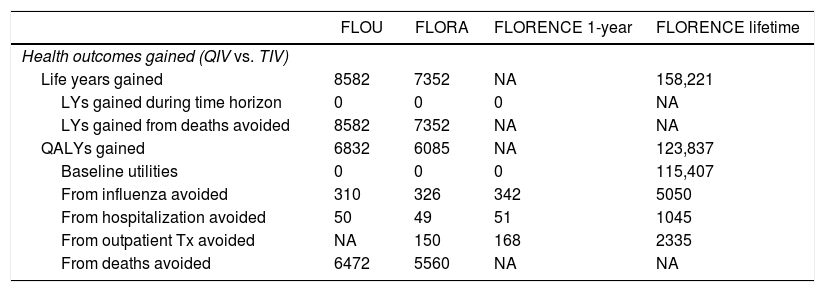
LYs and QALYs gained with QIV vs TIV in the models populated with best available data inputs.
| FLOU | FLORA | FLORENCE 1-year | FLORENCE lifetime | |
|---|---|---|---|---|
| Health outcomes gained (QIV vs. TIV) | ||||
| Life years gained | 8582 | 7352 | NA | 158,221 |
| LYs gained during time horizon | 0 | 0 | 0 | NA |
| LYs gained from deaths avoided | 8582 | 7352 | NA | NA |
| QALYs gained | 6832 | 6085 | NA | 123,837 |
| Baseline utilities | 0 | 0 | 0 | 115,407 |
| From influenza avoided | 310 | 326 | 342 | 5050 |
| From hospitalization avoided | 50 | 49 | 51 | 1045 |
| From outpatient Tx avoided | NA | 150 | 168 | 2335 |
| From deaths avoided | 6472 | 5560 | NA | NA |
QIV vs TIV, quadrivalent versus trivalent influenza vaccine; LY, life-year; QALY, quality-adjusted life-year; NA, not applicable; Tx, treatment.
The discounted cost per LY gained with QIV versus TIV was R$16,263 with FLOU, R$18,843 with FLORA (versus R$16,263 in Analysis 1), and R$15,072 with FLORENCE (versus R$18,000 in Analysis 1) using a lifetime horizon. The discounted cost-utility ratio was R$20,428 with FLOU, R$22,768 with FLORA (versus R$20,428 in Analysis 1), and R$19,257 with FLORENCE (versus R$22,490 in Analysis 1) using a lifetime horizon.
With increasing model complexity and using more detailed data inputs, the FLORA model produced less favourable results, while FLORENCE produced more favourable results for QIV. The key drivers of improved outcomes in FLORENCE with best available data inputs were all-cause mortality in healthy and at-risk individuals (with a 10-fold increase in mortality rate in at-risk individuals), adding antibiotics and associated costs, and finally providing more granularity in other inputs. The less favourable outcomes with FLORA, using best available data inputs versus using FLOU inputs were due to the 10-fold increase in mortality of at-risk individuals which led to shorter life expectancy of at-risk individuals, resulting in lower QALY gains and a higher cost per QALY gained.
DiscussionOne model type may be more appropriate than another, depending on the questions of the decision-maker. For example, in the case of influenza in Brazil, the FLOU model was able to provide an adequate estimate of QIV versus TIV cost-effectiveness in one year, including lifetime effects of premature mortality, with basic data and assumptions to fit broad age groups. FLORA was able to provide more insights about healthy versus at-risk populations, paediatric age groups within the population under 18 years old, as well as cost drivers linked to respiratory or non-respiratory complications. Finally, FLORENCE provided even greater certainty and precision than FLORA, adding details for age groups within the elderly population, more detailed cost and complication breakdowns, and the lifetime cost-effectiveness of consecutive annual vaccination.
The choice of a suitable model is therefore closely linked to the questions that will help decision-makers understand the value of the interventions being assessed. Another key factor to be considered, however, is the availability of data. The quality of the data that goes into the model has an impact on the quality of the outcomes; i.e., how closely they reflect the actual burden of disease and the true effect of interventions in the population. Economic models typically combine data on epidemiology, efficacy and safety, costs and resource use, to assess the impact on patients and society. It is not uncommon for models to rely on multiple assumptions as some data are often lacking. In this study, the model with the lowest data requirements was FLOU. However, even this model relied on assumptions (e.g., the proportion of the very young and elderly groups clinically at-risk) to fill data gaps for Brazil. Additional assumptions were required in the FLORA model (e.g., mortality risk in the at-risk versus healthy population were based on UK data), and in the FLORENCE model (e.g., probabilities of specific complications in each age group). While FLORENCE attempted to address issues related to broad age groups, using a 1-year horizon versus vaccination in consecutive seasons over lifetime, and oversimplification of lifetime effects, this model had some drawbacks. Age-stratified data to populate FLORENCE were sometimes limited, computing time to run sensitivity analyses took several hours/days, and as decision makers are more used to interpreting 1-year models, it may be difficult for health authorities to compare outcomes from this lifetime multi-cohort model.
This study has shown that when using the same base case data in all three models, despite differences in structural complexity, the models all provided comparable results; i.e., a cost per QALY ratio for QIV versus TIV of R$20,428 (FLOU and FLORA) and R$22,490 (FLORENCE). While this outcome validates the approach and assumptions made in the more complex models to some extent, it also shows that a less complex approach is able to satisfy the needs of decision-makers considering the available data. When comparing QIV and TIV, the driver of incremental costs was vaccination cost, and the driver of incremental QALYs was mortality. A back-of-the envelope calculation based solely on these parameters could provide an initial indication of whether the cost per QALY gained is within generally accepted willingness-to-pay thresholds, and if increased granularity in data inputs or model structure is needed. Key data sources (e.g., vaccine coverage and efficacy) should optimally match the model age-groups to avoid calculations and assumptions; i.e., the majority of data inputs for Brazil were reported for 0–4 and 5–17 years paediatric age groups and 18–49, 50–64, 65–74, 75+ years. The age groups for which data inputs are available and the desired level of accuracy in the results are thus drivers of which model to choose. The difference in all-cause mortality inputs between healthy and at-risk individuals was a critical driver of differences in outcomes between FLOU and FLORA. Hence, FLORA should be preferred over FLOU in case the difference between all-cause mortality is substantiated and well-documented.
In conclusion, a balance needs to be drawn between the level of detail and certainty of the answers required, and the ensuing level of complexity and data availability for the model. Of the many models assessing influenza vaccination, some offer more granularity than others but at a cost (i.e., loss of transparency with complex data requirements). In this study, the FLOU model provided transparency allowing decision-makers to better understand how the model works and what drives the outcomes. In addition, FLOU required less data and provided comparable results to FLORA and FLORENCE. All three models predicted a cost per QALY gained for QIV versus TIV in the range of R$19,257 (FLORENCE) to R$22,768 (FLORA) with the best available data in Brazil.
AuthorshipAll authors participated in the design or implementation or analysis, and interpretation of the study, and the development of this manuscript. All authors had full access to the data and gave final approval before submission.
FundingGlaxoSmithKline Biologicals S.A. funded this study (GSK identifier number HO-13-13962) and all costs related to the development of the manuscript.
Conflicts of interestThe company of LAVB and IVV received funding from GSK Group of Companies to complete the work disclosed in this manuscript. GTA declared to have received consultancy fees from GSK Group of Companies for the submitted work. AM and JG are employed by GSK Group of Companies and JG hold shares in the GSK Group of Companies.
References cited in the Appendices